Therefore, department management is responsible for ensuring all healthcare team members have adequate training in recognizing the symptoms, are familiar with pressure measuring equipment, and can escalate the situation appropriately and promptly. Implementing an interprofessional approach provides the best method for early detection to provide the best patient outcomes. The ability to escalate the situation in a timely fashion to a senior physician who can initiate early aggressive treatment with fasciotomy is crucial. These staff members need the most training in recognizing compartment syndrome and need to exercise a high index of suspicion. The hospital staff, typically attending physicians and nursing staff, has the most contact time with patients and is in the best position to detect increasing symptom severity. 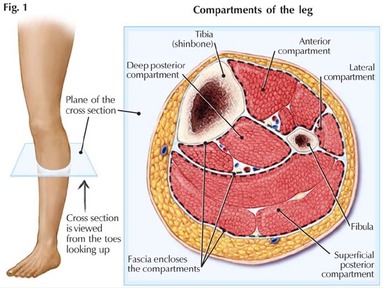
Įarly recognition of compartment syndrome is best detected by those professionals who have regular contact with the patients in the hospital. 
Ĭonsiderations of irreversible nerve and muscle damage and high risk of infection change the risk-benefit analysis in missed compartment syndrome and negate the necessity for emergency surgery. Patients who underwent a delayed fasciotomy had twice the amputation rate and 3 times the mortality rate. In a 2008 study, 336 combat patients received 643 fasciotomies (upper and lower limb included). The infection rate was significantly higher in patients with delayed fasciotomies. 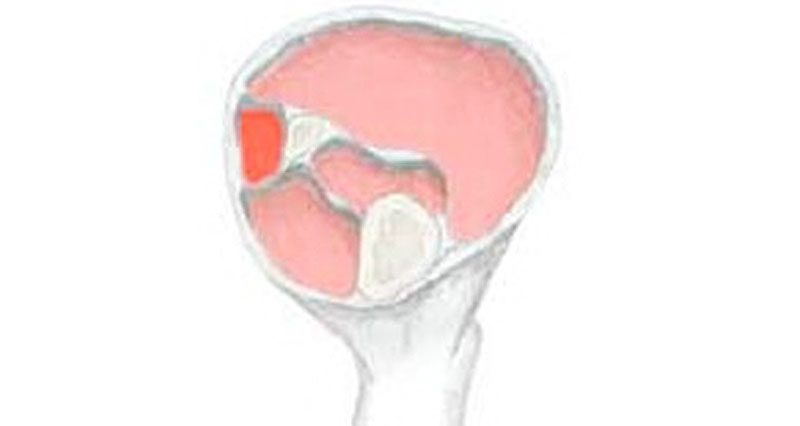
Conversely, another more recent study revealed no difference in limb salvage rate when comparing early (12 h) fasciotomy. However, fasciotomies performed after 12 hours resulted in only 8% of patients regaining normal limb function. One study demonstrated that fasciotomies performed within 6 hours resulted in almost complete limb function recovery fasciotomies performed between 6 and 12 hours resulted in a normal functional recovery rate of 68%. If the clinician suspects compartment syndrome has been present for more than 12 hours, there is a potential risk of reperfusion injury. The primary relative contraindication to performing a fasciotomy is delayed presentation. Every decision to perform an emergency fasciotomy should be made by a senior team member and on a case-by-case basis considering the patient's medical condition and the injury sustained. This section will explore the relative contraindications. Overall, 50% of patients reported being multisport athletes, according to results.No absolute contraindication to performing a fasciotomy exists. Researchers found 25% of patients reported running as their primary sport, followed by soccer (23%) and field hockey (12%). After the anterior and posterior compartments have been released, measure the pressure of the medial compartment. Results showed all patients presented with leg pain, with 5% reporting neurological symptoms and 85% presenting with bilateral symptoms that required bilateral compartment release. Make a 1- to 2-cm incision in the lateral intermuscular septum, and using Metzenbaum scissors, extend the septum proximally and distally along the length of the incision. Researchers recorded demographic and condition characteristics, operative procedure, postoperative course and clinical outcomes in 286 legs of 155 pediatric patients (88% girls) surgically treated for chronic exertional compartment syndrome (CECS) with compartment release. Recently published results showed 18.8% of patients experienced recurrent chronic exertional compartment syndrome, which more commonly occurred in pediatric patients who underwent anterior and lateral release only. If you continue to have this issue please contact to Healio 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
